During the first COVID-19 wave, when Saumitra Das and colleagues were sequencing thousands of samples every day to check for SARS-CoV-2 variants as part of INSACOG, they were racing against time to track mutations as they appeared. “If we wanted to predict whether one of these mutations was going to be dangerous from a public health perspective, we needed an assay system,” says Das, Professor at the Department of Microbiology and Cell Biology (MCB), IISc.
The assay protocol widely followed involved isolating the virus from the samples, creating multiple copies, and studying its transmissibility and efficiency at entering living cells. Working with such a highly infectious virus is dangerous and requires a Bio Safety Level-3 (BSL-3) lab, but there are only a handful of these labs across the country.
To address this problem, Das and his team, along with collaborators, and with funding from DBT, have now developed and tested a novel virus-like particle (VLP) – a non-infectious nanoscale molecule that resembles and behaves like the virus but does not contain its native genetic material.
Such VLPs can not only be used to safely study the effect of mutations that may arise in SARS-CoV-2 – without requiring a BSL-3 facility – but can also potentially be developed into a vaccine candidate that can trigger an immune response in our bodies. Soma Das, DST Woman Scientist in the Department of Biochemistry and one of the authors of the study, adds that these VLPs can also be used to cut down the time taken to screen drugs that can fight the virus.
Das’ lab has previously studied the Hepatitis C virus for 28 years, and shown that VLPs can be used as vaccine candidates. When the pandemic hit, they began working on a VLP for SARS-CoV-2. First, they had to artificially synthesise a VLP with all four structural proteins – spike, envelope, membrane and nucleocapsid. “The main challenge was to express all four structural proteins together,” says Harsha Raheja, PhD student at MCB and first author.
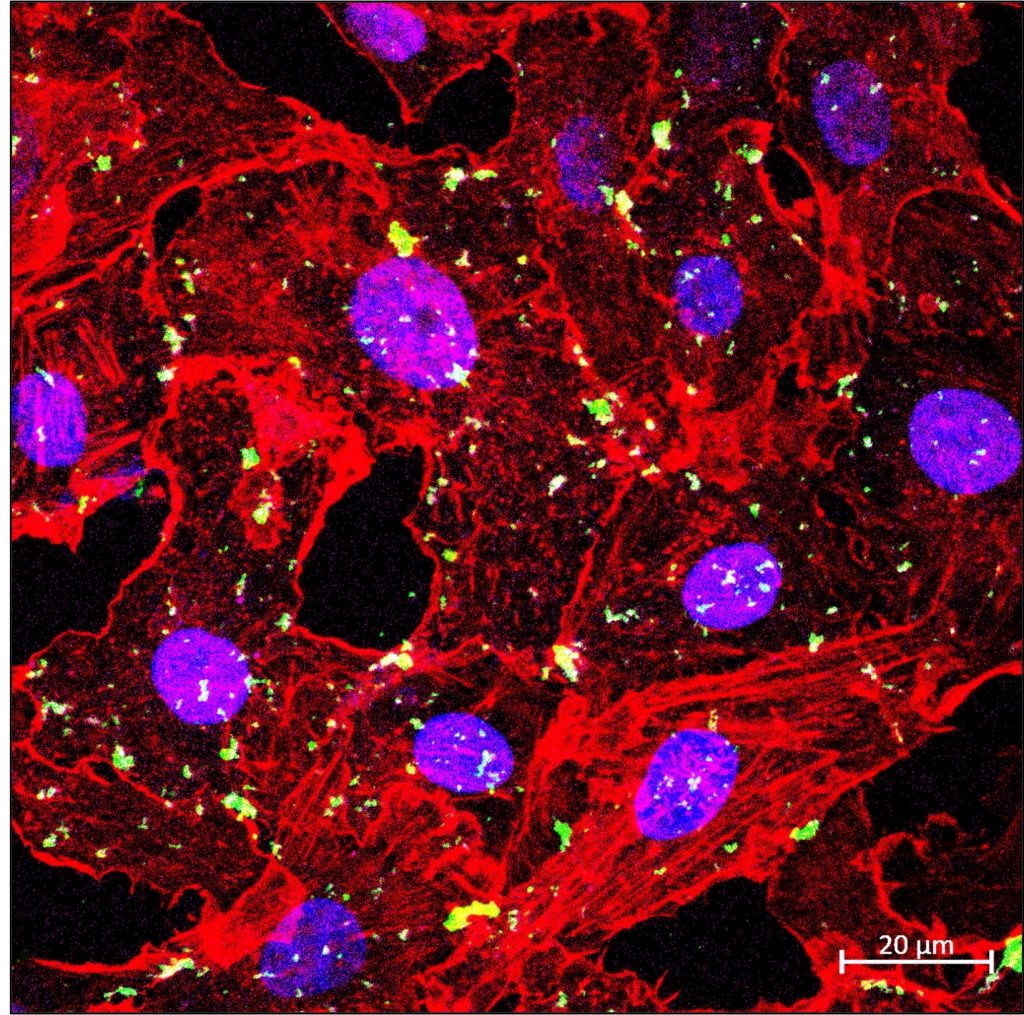
The team chose a baculovirus – a virus that affects insects but not humans – as the carrier to synthesise the VLPs, since it has the ability to produce and assemble all these proteins and replicate quickly. Under a transmission electron microscope, the VLP was seen to be just as stable as the native SARS-CoV-2. At 4 degrees Celsius, the VLP could attach itself to the host cell surface, and at 37 degrees Celsius, enter the cell.
When the team injected a high dose of the VLP into mice models, it did not affect the liver, lung, or kidney tissues. They also gave one primary shot and two booster shots to mice models with a gap of 15 days, after which they found a large number of antibodies generated in the blood sera of the mice. These antibodies were also capable of neutralising the live virus. “This means that they are protecting the animals,” explains Raheja.
The researchers have applied for a patent for their VLP and hope to develop it into a vaccine candidate. They also plan to study the effect of the VLP on other animal models (using the expertise of SG Ramachandra, one of the inventors), and eventually humans. Raheja says they have also developed VLPs that might offer protection against more recent variants like Omicron and other sub-lineages.