A team of undergrads is working on a solution for endometriosis as part of an international competition

It is early in the morning. The biology lab nestled within the old physics building at IISc echoes with hushed footsteps as a team of undergraduate students drop in one by one. After exchanging pleasantries, they don their white lab coats and check the assays of the previous day’s experiments. The results of the assay don’t look good, so they start the set of experiments from scratch again.
These experiments are not required for their regular coursework. The project that these students are working on is part of international Genetically Engineered Machine (iGEM), a synthetic biology competition that brings together high school, undergraduate and graduate students from different parts of the world to compete against each other for awards. Student teams from the participating colleges design, test and develop tools using advanced synthetic biology techniques. The IISc team participating this year is working on designing a therapeutic solution for endometriosis.
Endometriosis is a painful disease that affects approximately 10% of all women who are of reproductive age worldwide, according to the World Health Organisation. In a healthy person, every month, an inner lining called the endometrial tissue grows to help prepare the uterus for pregnancy. During menstruation, that lining is shed. However, in a person with endometriosis, this tissue gets lodged outside the uterus, and reacts to the hormones that trigger bleeding and shedding. This results in the formation of lesions, cysts, nodules, and scar tissue that causes severe cramping, bleeding, and pain.
In the human body, any excess tissue that grows where it shouldn’t, gets cleared out by macrophages – immune cells that destroy such excess tissues as well as bacteria and other harmful organisms. But in endometriosis, the macrophages secreted by the uterine layer to clear up these tissues don’t do their job. Instead, they produce proteins like interleukin-8 (IL-8) to signal another immune taskforce called neutrophils, which then call for more macrophages. “It’s like a vicious cycle,” says Aditya Kamath Ammembal, a BSc (Research) student at IISc and this year’s iGEM team leader.
The IISc iGEM team’s project aims to use short stretches of genetic material called messenger RNAs (mRNAs) coding for an antibody against interleukin-8 to block the same in the disease tissue. But their search for a solution was not straightforward.
The search for a cure
Aditya explains that the team initially started looking at exosomes – nanosized structures secreted by some cells – as vehicles to deliver a stretch of genetic material called micro-RNA into the macrophages. But after talking to PhD students and faculty members, they realised that the specific region they were looking at in fibronectin – one of the molecules in the disease tissue – was difficult to target with the resources at hand.
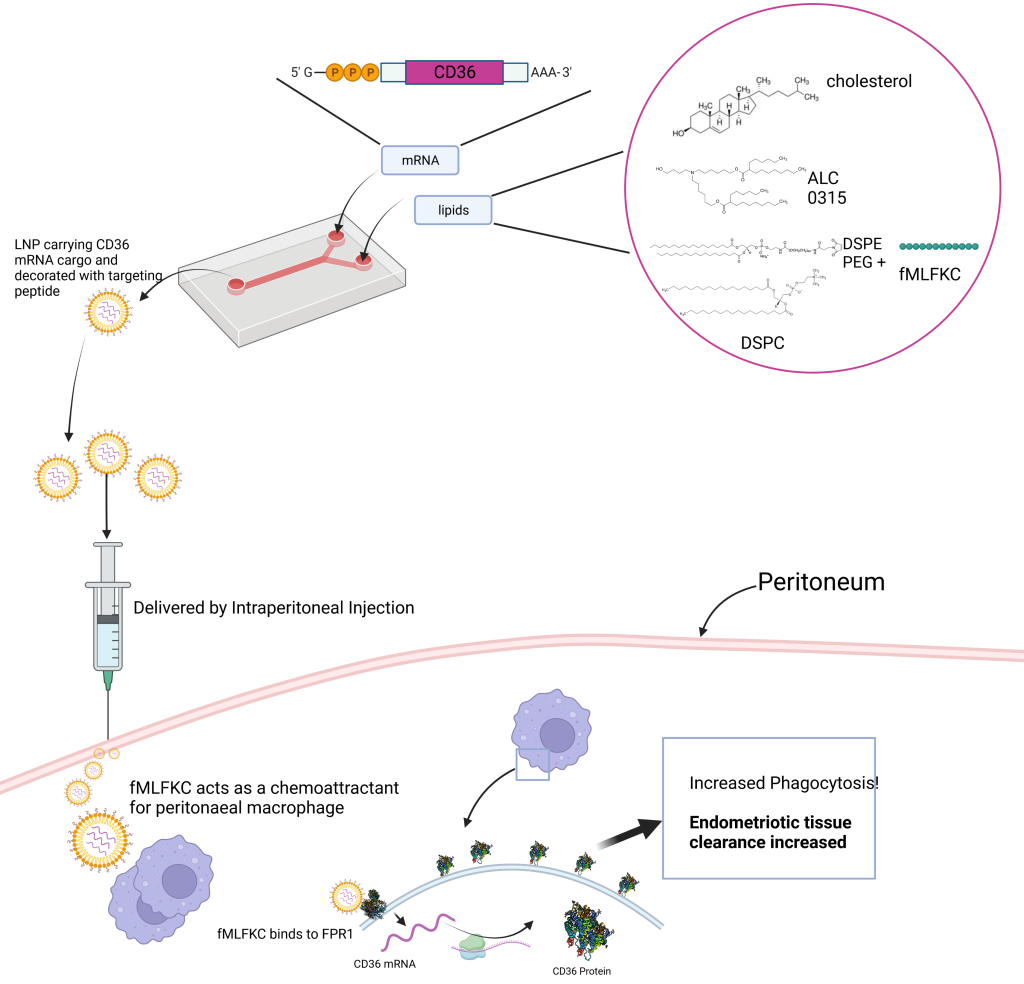
After speaking to Rachit Agarwal, Assistant Professor at the Department of Bioengineering, the team decided to explore a lipid nanoparticle (LNP) delivery system which could shuttle mRNAs (which are different from micro-RNAs) into the cell effectively. In the human body, mRNAs are the precursors that “code for” and kickstart the production of specific proteins or antibodies. When they are artificially stitched together in the lab and inserted into a cell, they can nudge the cell to produce the antibody they code for.
Around the same time, the team found out about aptides – short peptide chains that can help home in on specific cells. They decided to decorate the surface of their LNP with these aptides so that they can accumulate at the disease site: the excess endometrial tissue. After sifting through literature reviews to figure out which protein would be the best target, the team came across IL-8. “We realised that blocking IL-8 would probably produce the most favourable results,” Aditya explains. Blocking IL-8 locally could stop other macrophages from accumulating near the tissues, breaking the cycle. Therefore, the team designed an mRNA that could nudge cells to produce an antibody which blocks IL-8.
The team also found that in patients with endometriosis, the defective macrophages don’t produce enough of a protein called CD-36 that sits on their membrane. If another piece of mRNA could be used to boost CD-36 production, then these macrophages could probably clear excess endometrial tissue better.
The team’s therapy, therefore, combines these twin approaches: Designing artificial mRNAs ensconced in aptide-studded LNPs to both block IL-8 in the tissue, as well as boost CD-36 production in the macrophages.
But when the team spoke to doctors and other researchers, they realised that since mRNA gets degraded and does not stay inside the cell forever, it needs to be repeatedly administered. Therefore, the team is now in search of a more permanent fix. They are planning to see if proteins produced by the mRNAs shuttled into the target cells can somehow be recycled. “Membrane proteins in general are recycled because their production is very energy expensive,” Aditya elaborates.
The next step would be testing the effects of these mRNA therapeutics on endometrial tissue cell lines. The team is also planning to collaborate with Ramray Bhat, Associate Professor at the Department of Developmental Biology and Genetics (DBG), to develop an organ-on-chip prototype – a mechanical setup that will recreate the effects of their therapy on specially designed spheroids made of endometrial cells in the lab.

Beyond the lab
There are other aspects to the iGEM project apart from the research. The students also devote a lot of time to spreading awareness about the topic – in this case, endometriosis – and talking to stakeholders like industry experts, researchers, and doctors who might ultimately administer the therapeutic solution to the patient. Apart from slogging away in the lab every day, the team has also taken up many outreach initiatives.
For example, while carrying out the project, the team noticed that a lot of materials for the research – like cell lines – had to be imported from other countries like the USA. This meant that materials took longer to get delivered and the delivery charges added 20-30% more to the product price. But if the product is manufactured in India, it could be transported quickly, and the costs would be lower. The team also started a campaign for a ‘National Biotechnology Day’ in India to spread awareness about the field and its impact. They collected email addresses of researchers at various biotechnology universities across India and requested them to support the campaign. In addition, the team is working on raising funds to buy essential software and testing kits, and for their awareness campaigns.
IISc teams have participated in iGEM for several years and have won gold medals five times. The current iGEM team intends to pass on a module of some kind – a set of guidelines to help future iGEM teams at IISc. This module would contain data from the previous team’s research, models and resources they used, and most importantly, a guide on how to read and understand research papers. This is because the teams are comprised of students from both biology and non-biology backgrounds – which was the case for Sanika Amol Borade and Mrigank Pawagi, who are pursuing a mathematics major in the BSc (Research) and the BTech programme respectively. Both agree that it was difficult to understand research papers initially and the ideas discussed flew over their heads, but over time they have come to understand and appreciate the subject a lot more.
In addition, the team hosted a science camp for middle and high school students, where they discussed synthetic biology, biosafety, and endometriosis. They conduct regular webinars where experts are invited to talk about the disease. The team has also designed a mascot called ‘Lipi Di’ named after the lipid nanoparticle that is at the heart of their therapy.
Crucially, the iGEM team is keen on understanding the demand for such a therapy in the market and developing a business model in partnership with pharma companies for commercialising it. Yukta Subramanian, a BSc (Research) student and one of the team members, says, “We plan to take this beyond the lab and help people.”